Using Evoked Potentials to Build a Clinical Picture in Adults- Guest Blog
Case report by Jason Smalley, Specialist Audiologist,
Jason is a Specialist Audiologist at Nottingham University Hospitals, specialising in the Evoked Potentials Assessment of all ages and currently sits on both the Evoked Potentials Special Interest Group of the BSA and on the clinical advisory group of the Newborn Hearing Screening Programme for England.
Evoked Potential (EP) testing has become embedded into our paediatric clinical practice, whether that is auditory brainstem responses (ABR) on infants at birth or Otoacoustic responses performed to back up behavioural testing. Fewer departments however use other forms of evoked potentials such as cortical response testing (CERA) or neurological ABR (nABR) to build up a clinical picture of the adult auditory system, particularly within complex adult patients despite their ability that when considered together, they can pinpoint a site of lesion and assist with management. 2 clinical case studies are presented where the use of EP allowed a problem to be identified which otherwise might have been missed.
Case 1:
A 31-year-old male was referred from ENT into adult audiology. He had been working as a trust interpreter and spoke 4 different languages; however he felt his hearing had been declining for some time, and he was now struggling in background noise and groups of people. There was no significant medical history and he initially presented with a flat bilateral 40 – 50dB sensorineural loss. He was recommended hearing aids and fitted bilaterally with hearing aids.
At follow up, he reported still being unable to hear well with the hearing aids. After several adjustments and appointments where he would still express that speech wasn’t clear / he was still struggling, he was referred for further investigation.
Initial investigation revealed peaked 226Hz tympanometry bilaterally with present transient evoked OAEs bilaterally at 1.4, 2.0 and 2.8kHz (based on a signal to noise ratio of 6dB), Figure 1.
2 channel Cortical testing (figure 2) was performed which showed cortical thresholds consistent with the pure-tone audiometry detection thresholds but not consistent with the present TE-OAEs (60dBHL right 4kHz, 40dB HL left 4khz, 40dBHL bilaterally at 1kHz).
Neurological ABR was then performed using initially a 90dBnHL alternating click stimulus before raising to 100dBnHL bilaterally. This showed no ABR like response to sound. 4kHz and 1kHz tone pip ABR was then performed to 105dBnHL at 4kHz and 100dBnHL at 1kHz – for ease only some of these traces are shown in figure 3. This showed again, no ABR like response to sound.
These results are entirely consistent with Auditory Neuropathy Spectrum disorder and the adult was referred for a neurological opinion.
Case 2:
A 42 year old lady was referred urgently to ENT as she was ‘unable to hear anything with query sudden loss in both ears’.
They were seen in ENT clinic the following day and produced an audiogram consistent with a profound bilateral sensorineural hearing loss, however robust TE-OAE’s were present in both ears. Whilst starting steroid treatment, the ENT doctor also referred the lady for EP testing to work out a root cause.
At EP testing, again, strong TE-OAEs were seen bilaterally (figure 4) and so neurological ABR was performed bilaterally using an 80dBnHL alternating click stimulus and headphones. This revealed normal ABR like waveforms with all peaks within inter-peak and absolute normal range (figure 5).
Cortical testing was then performed, however this was consistent with the profound pure tone audiometry, with thresholds around 100-120dB bilaterally at 2 and 4kHz (figure 5). Following discussion with ENT medic that this looked like a central loss, the lady was referred for urgent MRI scan, where it was found that a transient ischaemic attack had likely taken place which had affected both hemispheres of the auditory cortex. The lady was referred to the cochlear implant team for an opinion and now has a non-spoken language communication strategy.
Conclusion: By using different auditory evoked potential testing on complex patients we can build up a clinical picture of where an issue may be and so support the patient better with management.
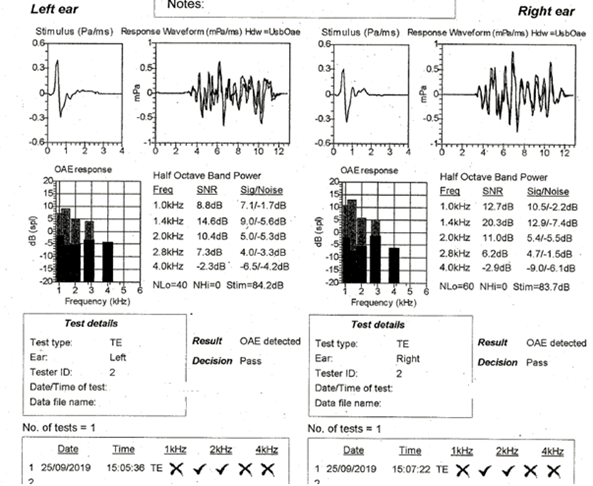
Figure 1
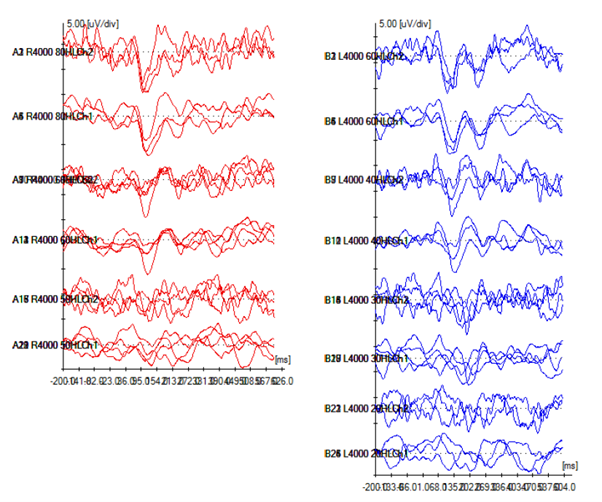
Figure 2
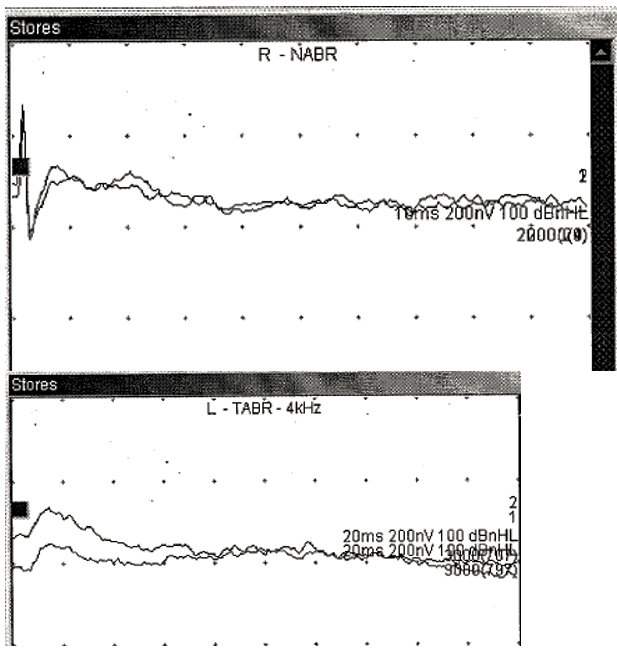
Figure 3
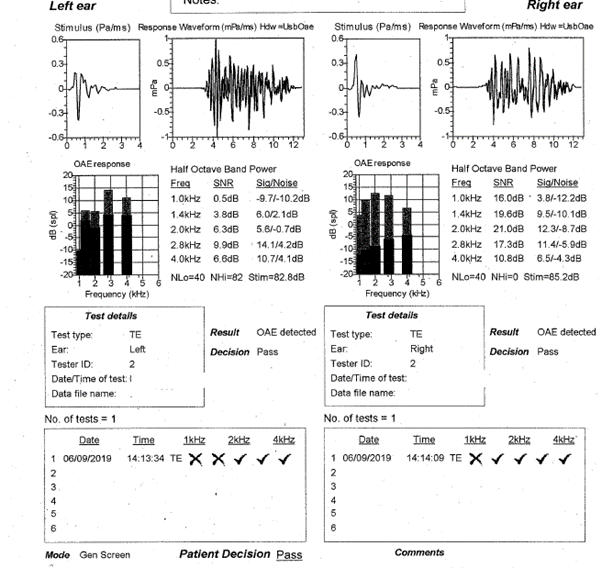
Figure 4
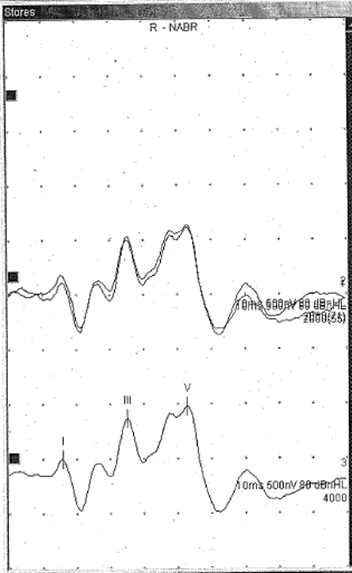
Figure 5
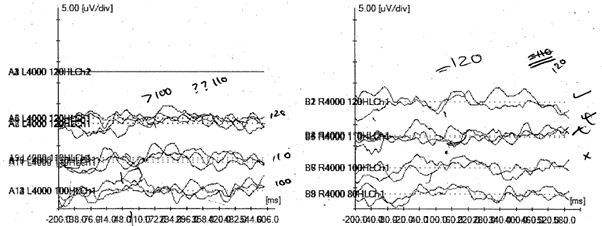
Figure 6









